 During my 30-year journey in eye surgery, no story has been as dynamic and exciting as the story of the human eye natural lens, its disorder called cataract, and our relentless effort to improve the process by which the cataract is evacuated and replaced with a man-made intraocular lens, and to fine tune the materials and the design of the intraocular lens implant that we place in the eye when we remove the cataract.
During my 30-year journey in eye surgery, no story has been as dynamic and exciting as the story of the human eye natural lens, its disorder called cataract, and our relentless effort to improve the process by which the cataract is evacuated and replaced with a man-made intraocular lens, and to fine tune the materials and the design of the intraocular lens implant that we place in the eye when we remove the cataract.
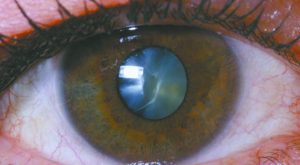
The story begins here. The human eye has a lens that sits behind the pupil that inspired the design of the camera with a lens behind the shutter. This lens is made up of a protein similar to egg white: when it is fresh it is transparent and when you cook it, it clouds up. With time the protein that makes up the human natural lens “cooks”, a cataract develops, and our vision suffers. The young natural lens is a creative marvel: it focuses at distance and very quickly can zoom close up to a clear image that is devoid of unwanted optical aberrations. However, as the natural lens ages it begins to lose some of its remarkable capabilities in a process called the dysfunctional lens syndrome (DLS). This syndrome begins with the gradual loss of accommodation (zoom) due to the loss of the natural lens elasticity that is typically first noticed around age 40 and eventually mandates the use of reading glasses. DLS progresses as the lens begins to lose its transparency and some unwanted optical phenomena emerge such as glare and halos but the vision overall remains “good enough” with glasses. Some people at this point elect to have a highly successful procedure to replace the dysfunctional natural lens with a multifocal lens implant to resore their ability to see without glasses. Eventually the lens becomes cloudy enough that it affects the person’s ability to carry on his or her activities of daily life: this cloudiness is what we call cataract. At this point, the changes in the lens are deemed medically significant and the person may elect to have insurance based cataract surgery. Cataract surgery in a nutshell is a procedure in which the old dysfunctional cloudy natural lens is replaced with a man-made intraocular lens IOL.
This IOL has come a long way since its inception some Eighty years ago. The first models of these lenses where rigid and optically low tech. Today’s IOLs are by far some of the most technologically advanced marvels and are generally divided into two basic groups. The first is an IOL that is monofocal: it corrects the vision at distance but the patients still requires reading glassed. The second id a multifocal IOL that is typically designed to focus at distance and near and can reduce or eliminate entirely the need to wear glasses for any visual tasks.
This multifocal group has a number of different types: some are most suitable for golfers and active outdoors types, others for serious cell phone and computer users and others for avid small print readers. It is particularly crucial to match the person with the type of lens implant that most fulfills his or her visual requirements.
The field of intraocular lens implants is crowded with numerous offerings. I tell patients that there are many shapes and models of lens implants just as there are many different models of cars on the highway: putting the best implant in the patient’s eyes that best fit his or her visual demands guarantees a comfortable “ride”.
Intraocular lenses differ in rigidity ( rigid versus flexible), whether they are one or three pieces, whether they are made of silicon or acrylic or some other material, whether they are spherical or aspherical, and whether they are monofocal or multifocal. These offerings are wonderful in the sense that at the time of surgery we can pick out the lens implant that best matches the patient. For instance, patients with potential retinal problems are not suitable for silicon implants because if ever they needed retinal surgery requiring the use of silicon oil, the presence of a silicon implant affects overall visualization. Whereas multifocal implants are a technological wonder, giving most patients the ability to see distance and near without glasses, they are not suitable for everyone. For example I do not use multifocal implants in patients with macular degeneration or diabetic retinopathy because such patients will not reap the full benefits of such implants and single vision implants may offer such patients better quality vision. I perform cataract surgery one eye at a time not only as a precaution against infections as these have become quite rare with modern facilities and techniques, but also because when the first eye is done, we obtain measurements after the surgery that we take into account when performing the surgery on the second eye to insure that both eyes work optimally to give the patient the best vision possible.
Few patients ever ask me what implant I plan to use for them when I perform their cataract procedure in terms of material and design. However, I have tried through my writings, lectures, and patient care to increase awareness of implant differences, as I believe truly that the more informed the patient is, the better choices they will make for his or her eye health. We ophthalmologists are some of the most detail oriented professionals as our world is not measured in feet or inches but in microns. When that quality is combined with a well-informed eager-to-learn patient the result are good choices that make the patient very happy and rewards the ophthalmologist as he or she see that the fruit of their long years of education and training is making a positive difference in the world.
Florida Eye Specialist Institute
352.237.0090
Check Also
CUSTOMIZABLE LIGHT ADJUSTABLE LENS A GAMECHANGER FOR CATARACTS PATIENTS
All Americans have some degree of cataract change by the age of 75. As the …
 Central Florida Health and Wellness Magazine Health and Wellness Articles of the Villages
Central Florida Health and Wellness Magazine Health and Wellness Articles of the Villages