By Patricia Spitzer, PA-C – Village Dermatology & Cosmetic Surgery, LLC
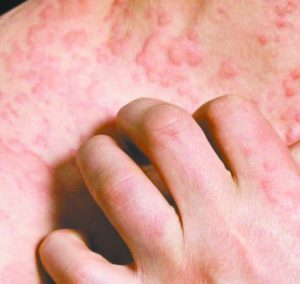 According to the National Association of Eczema there are over 13 million people that suffer with eczema, so there is a good chance you or someone you know has been affected. The term eczema is broad and as a general definition we refer to something as eczematous when it becomes dry, red or cracked. The overall presentation of eczema varies widely but there are three distinct stages based on timing; acute, subacute and chronic. There are multiple different types of eczema including irritant or allergic contact dermatitis, stasis dermatitis, atopic dermatitis, nummular eczema, dyshidrotic eczema, hand eczema, eyelid dermatitis, seborrheic dermatitis, lichen simplex chronicus, etc.. Each one of these conditions has a different cause and presentation but they have a commonality in that the skin is red, itchy and dry.
According to the National Association of Eczema there are over 13 million people that suffer with eczema, so there is a good chance you or someone you know has been affected. The term eczema is broad and as a general definition we refer to something as eczematous when it becomes dry, red or cracked. The overall presentation of eczema varies widely but there are three distinct stages based on timing; acute, subacute and chronic. There are multiple different types of eczema including irritant or allergic contact dermatitis, stasis dermatitis, atopic dermatitis, nummular eczema, dyshidrotic eczema, hand eczema, eyelid dermatitis, seborrheic dermatitis, lichen simplex chronicus, etc.. Each one of these conditions has a different cause and presentation but they have a commonality in that the skin is red, itchy and dry.
Terms associated with Eczema: Dermatology can be its own language and it’s important to understand some of the most common terminology associated with eczema.
Pruritus: itching
Xerosis cutis: generalized dry skin
Lichenification: thickening of the skin typically due to chronic friction or scratching
Erythema: Redness
Dermatitis: irritation of the skin
Excoriation: Scratches
Causes:
It’s hard to pinpoint an exact cause of eczema as there are a multitude of factors that lead to an eczematous exacerbation. Below is a list of the most common causes that are seen in practice.
• Hereditary – if both parents have a history of eczema the child is likely to have a history as well
• Chemical irritants – abrasive chemicals that strip the natural oils of the skin leading to drying and irritation
• Allergens – Food, environmental
• Water Exposure – too much water exposure leads to drying
• Temperature extremes
• Stress/anxiety – can have a negative effect on the immune system and this has been proven to cause several of the eczematous processes dermatologist treat
Atopic Dermatitis:
This is the most common form of eczema and refers to a condition that is typically seen in children but can occur in any age group. It has been referred to as the itch that rashes. The reason behind that saying is due to a chronic itch-scratch cycle, the more we scratch at the skin the worse it gets and the thicker that patches get. We do not know the exact mechanism that drives this condition but we are aware that there is a hereditary component coupled with environmental triggers. The typical presentation is to the cheeks in infants, flexural surfaces, such as the inner elbow, back of the knees, neck and eyelids in children 2 years and older. The presentation in adulthood various widely but seems to have a worse prognosis in terms of chronicity. Allergies, asthma and atopic dermatitis typically go hand in hand and this is referred to as the atopic triad. There is a strong correlation with allergies to foods or environmental factors that cause exacerbations of atopic dermatitis. As research into Atopic Dermatitis continues there are more and more treatment modalities coming into play, especially in the immunologic department.
Preventative measures?
It’s important to avoid anything that dries the skin as this will further exacerbate or possibly bring on an episode of eczema.
• Avoid abrasive soaps or chemicals as these dry out the skin and can cause irritation leading to itching or cracking of the skin. In practice, I currently recommend products that are gentle and liquid soap versus bar soap to avoid scrubbing.
• Counterintuitive to thinking, it’s important to avoid water exposure for any prolonged length of time, especially hot water as this can be a driving factor for exacerbating dry skin.
– Some of the recommendations for those with children or who are suffering from eczema personally short, warm or cool showers or baths are recommended and for pool exposure it’s important to specifically limit the duration of the swim as well as make sure to put an emollient such as Vaseline or Aquaphor to wick away the water in areas that are known trouble spots.
• Avoid known food or environmental triggers
• Make sure to use a moisturizer daily on damp skin to enhance penetration
• Avoid scratching or rubbing dry, itchy areas as this can make the condition worse
So what’s the bottom line here? Eczema is a very common condition, in fact, the most common cause of inflammation of the skin. There are several ways to prevent exacerbations, such as the use of moisturizers daily, avoiding known triggers and prolonged water exposure especially to hot water and most important do not scratch! If this doesn’t work then it might be time to go to your local Dermatology office for evaluation and treatment.
Treatment modalities:
The treatment of eczema varies widely. For skin that is more xerotic than inflamed the aim is more toward prevention and moisturization with products such as CeraVe, Cetaphil, Vanicream or Amlactin. When the skin becomes pruritic and erythematous a topical steroid is the treatment of choice on the trunk and extremities, but when the face or thinned skin areas are involved topical immunomodulators are preferred. Antibiotics are typically only prescribed when there is evidence of a secondary infection, usually due to staph found under the fingernails when scratching. Of course, depending on the severity and nature of the condition there are other specific treatments that may be required such as anti-histamines, oral steroids, immunologic medications, etc.
Village Dermatology
352-751-6565 | www.villagederm.com
1950 Laurel Manor Drive
Building 220—Suite #224, The Villages, FL 32162
Check Also
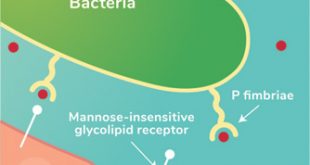
Recurrent UTIs: Addressing the Risk of Antibiotic Resistance
Urinary tract infections (UTIs) are common bacterial infections that affect millions of individuals worldwide each …
 Central Florida Health and Wellness Magazine Health and Wellness Articles of the Villages
Central Florida Health and Wellness Magazine Health and Wellness Articles of the Villages