 Lumbar Spinal Stenosis (LSS) is a narrowing of the spine that produces undue pressure on the nerves. Although younger people can experience stenosis through genetic mutations or from traumatic injury, it is more common in the aging population. Our vertebrae begin to be less lubricated with age, and they no longer protect the discs the way they were intended to do so. The lumbar portion of the spine is the lower part of the back that curves inward. It’s connected to the thoracic and the sacral region of the spine. Narrowing of the spine can occur anywhere, but when it affects the lumbar region, it disturbs significant mobility issue for many people.
Lumbar Spinal Stenosis (LSS) is a narrowing of the spine that produces undue pressure on the nerves. Although younger people can experience stenosis through genetic mutations or from traumatic injury, it is more common in the aging population. Our vertebrae begin to be less lubricated with age, and they no longer protect the discs the way they were intended to do so. The lumbar portion of the spine is the lower part of the back that curves inward. It’s connected to the thoracic and the sacral region of the spine. Narrowing of the spine can occur anywhere, but when it affects the lumbar region, it disturbs significant mobility issue for many people.
Symptoms
• Back pain
• Leg pain
• Burning pain in buttocks/legs (sciatica)
• Weakness and tingling in the legs, buttocks,
and feet
• Rigidity and stiff thigh muscles
• Foot drop/slap sensation when walking
• Incontinence
There are multiple options for treatment, and talking with your doctor about the right method for you is critical. Nonsurgical treatment will not correct the narrowing of the spine, but it can offer relief from discomfort and pain. Surgical treatment is usually reserved for difficult cases that are affecting the patient’s quality of life.
Nonsurgical Treatment
• RF denervation
• Regenerative Treatments (stem cells and exosomes)
• Physical therapy
• Anti-inflammatory medications. Non-steroidal
anti-inflammatory drugs (NSAIDs)
• Steroid injections (corticosteroids)
• Pain medications
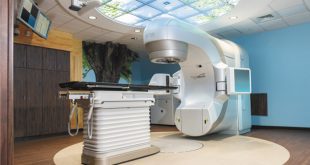
Minimally Invasive Treatment:
The mild® Procedure
Dr. Panchal with the National Institute of Pain is one of an elite group of physicians trained to use the mild® spinal stenosis procedure.
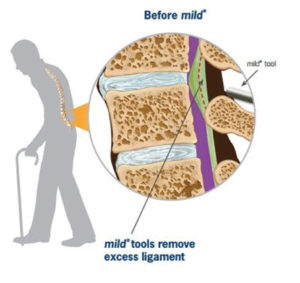
Vertos Medical explains the procedure in this way, “The mild® procedure treats LSS by removing hypertrophic ligamentum flavum, which helps restore space
in the spinal canal. The restoration of space reduces pressure on the nerves, reduces pain, and improves mobility. The procedure is performed through a 5.1 mm treatment portal via a posterior approach using live fluoroscopy. This method and the mild® instruments are designed to debulk tissue while maintaining the integrity of the ventral fibers of the ligamentum flavum by staying posterior to the thecal sac.1
“The epidurogram is a key safety feature since it allows the physician constant visualization of the treatment area throughout the procedure. Another key safety feature is the minimally invasive design of the procedure itself, which requires no general anesthesia, no implants, no stitches, and is performed in about one hour.
“mild® has been performed on over 20,000 patients and has been proven to be safe and effective in 13 clinical studies and more than 20 peer-reviewed journal articles. Clinical trials demonstrate that mild® can help LSS patients stand longer and walk farther with less pain2 and no major device-related complications have been reported.3
“A doctor who is certified to perform mild® will use an imaging machine and specialized tools to remove small pieces of bone and excess ligament tissue through a tiny incision in your back. Removing these elements restores space in the spinal canal and decreases the compression of the nerves, which reduces pain and restores mobility. Some doctors have described the goal of the procedure as being similar to removing a kink in a drinking straw. The outpatient procedure is typically performed in less than 1 hour. Patients are able to resume light activities within just days and requires no general anesthesia, no implants, and no stitches.”
References
1. 2012 data from Health Market Sciences report for Vertos Medical 2013.
2. Mekhail, Nagy, et al. (2012) Functional and Patient-Reported Outcomes in Symptomatic Lumbar Spinal Stenosis Following Percutaneous Decompression. Pain Practice, 12(6): 417–425. doi: 10.1111/j.1533-2500.2012.00565.x.
3. Based on mild® procedure data collected in all clinical trials.
The National Institute of Pain utilizes the most advanced, innovative methods from radiofrequency to spinal stimulation to treat pain from surgical complications as well as the following:
• Back and neck pain, including herniated discs, spinal stenosis, tumors and fibrositis.
• Cancer Pain.
• Neuropathic Pain.
• Complex regional pain syndrome (also known as reflex sympathetic dystrophy or RSD.
• Muscle and joint pain.
• Disorders of the nervous system, including shingles and trigeminal neuralgia (facial pain).
• Chronic abdominal pain and pelvic pain.
• Pain from traumatic injuries including auto accidents
• Pain associated with osteoporosis and vertebral compression fractures.
• Sports related injuries.
At the National Institute of Pain, they treat each patient individually, using the latest equipment and various innovative procedures to diagnose pain and determine your care needs. The National Institute of Pain’s President and Founder, Dr. Sunil Panchal, is a board-certified pain management physician.
Dr Panchal has held leadership responsibilities in many professional societies, including the Committee for Pain Medicine for the American Society of Anesthesiologists. Dr Panchal has authored and co-
authored a number of abstracts, journal articles, and book chapters. He currently serves as an invited editorial reviewer for Clinical Researcher, Anesthesia and Analgesia, Pain, Pain Medicine, and the Clinical Journal of Pain. He previously served as Editor-in-
Chief of the International Journal of Pain Medicine and Palliative Care and of Seminars in Pain Medicine. Dr. Panchal also served as the Chair of the National Comprehensive Cancer Network Cancer Pain Panel and has lectured widely at the national and international level. He is actively involved in the development of novel analgesics and neurostimulation devices, and in clinical research protocol design.
At The National Institute for Pain, their goal is to strive to deliver the highest quality of comprehensive care for those who are suffering from acute and chronic pain. They have many alternatives to help you with your personalized pain management needs. Please visit their website at www.nationalinstituteofpain.org or call them at (813) 264-PAIN (7246).
Check Also
Revolutionizing Healthcare: Exploring Regenerative Medical Treatments at QC Kinetix
By Daniel Sucherman, MD In recent years, the field of regenerative medicine has emerged as …
 Central Florida Health and Wellness Magazine Health and Wellness Articles of the Villages
Central Florida Health and Wellness Magazine Health and Wellness Articles of the Villages