By Brenda Superko, RN
The COVID-19 pandemic, to date, has claimed more than 450,000 lives globally with 118,000 lives lost in the United States. It has triggered a 21st Century quarantine order aka ‘shelter in place’, which was followed by our nation’s highest unemployment since the Great Depression. Early in the headlines surrounding the COVID-19 pandemic, we learned of the critical need for testing. The White House Coronavirus Task Force, as well as Infectious Disease experts, emphasized that testing was key to community mitigation strategy. The demand for testing was so critical that an Emergency Use Act was required by the Federal government to provide testing development and mass production. However, rapid and mass test production met significant hurdles with supply-chain issues. The chemicals necessary to perform testing, and even the swabs themselves, are mostly produced over-seas. Global competition and shipments from foreign ports soon became the next unforeseeable bottle neck to our nation’s urgent need for testing. And not unlike other medical laboratory tests, the true value rests in comprehending the results and its interpretation moving forward.
COVID testing and one’s understanding of the results has serious and consequential implications for the community as well as the individual.
There are 2 categories of laboratory tests: one that detects evidence of the virus and the other that detects antibodies formed in the blood in response to the virus. The virus (SARS-CoV-2) has its own very specific genetic material and thus the testing relies on detecting that specific genetic code in the collected specimen. Even with advanced laboratory science today, testing for the virus is heavily reliant on obtaining a specimen that has enough of the virus for the test to detect. It is possible that a test result could be inaccurate due to poor specimen collection, improper handling of the specimen or even early stage of the virus and therefore not enough of the virus in the specimen for the test to pick up. It is possible to have a “not detected” result on the virus test yet you still have the virus in your body. This is called a false negative test and is why the test results must be interpreted along with physical signs and symptoms of a virus infection.
The antibody testing indicates immune response to the virus and can provide evidence of prior exposure. The antibodies most relevant in reporting the status of a SARS-CoV-2 virus exposure are Antibody IgM and Antibody IgG. Serum lgM indicates recent infection and is typically positive within 3 to 10 days of symptom onset, whereas serum lgG is often present within 1 to 2 weeks from symptom onset and plateaus around 3 weeks, indicating current or past infection. Timing of these tests is a very essential step to community mitigation and determining contagion.
First, the virus test can tell you if the virus is currently present in your body and if you are at risk of passing it on to other people.
Second, the IgM antibody blood test can indicate that your immune system responded to a virus attack in the recent past since it tends to increase approximately 7 days after you are first exposed to the virus and is pretty much gone around 21 days after you first contact the virus. Thus, elevated IgM blood antibody levels suggest a recent infection.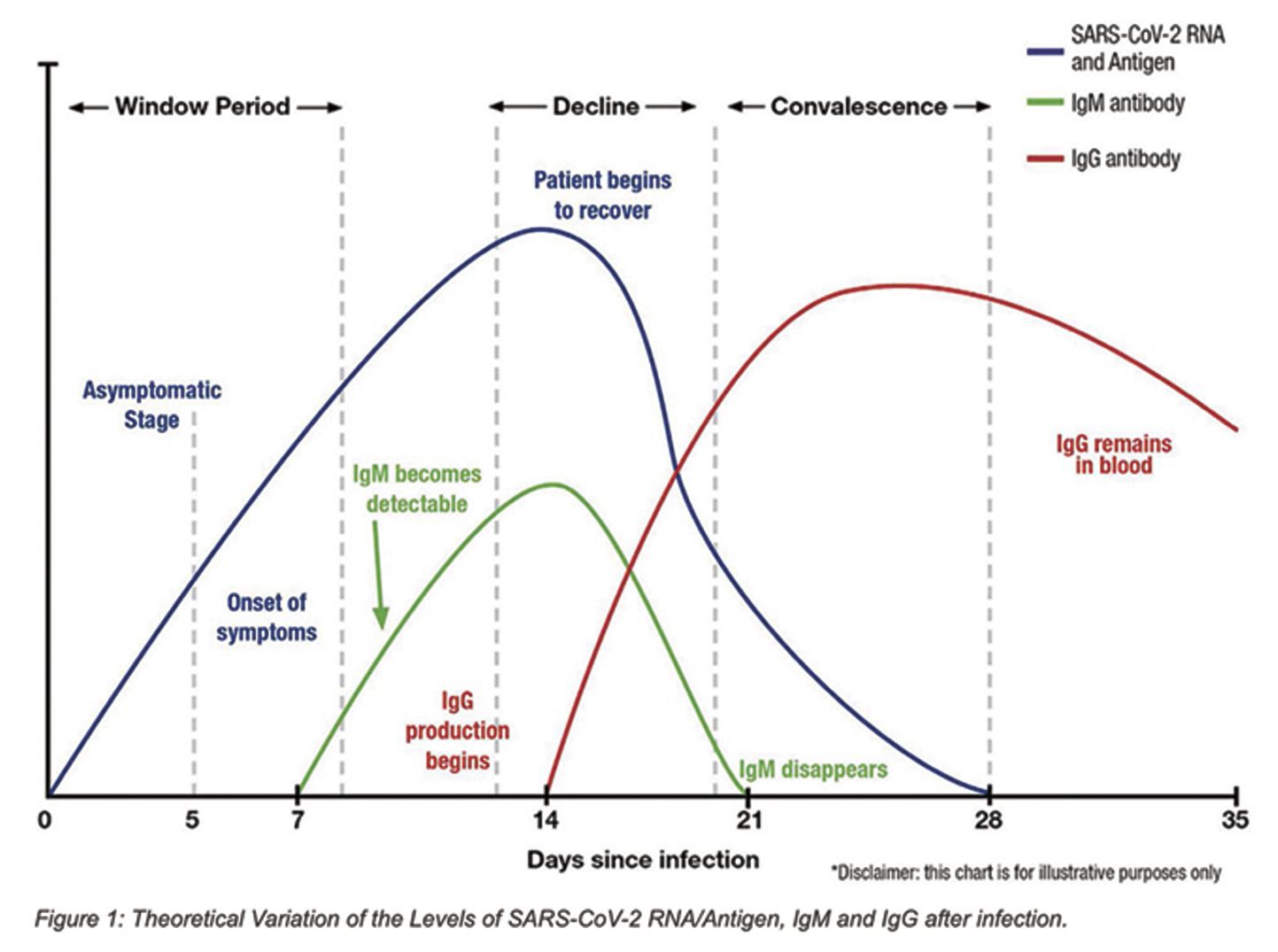
Third, the IgG antibody blood test is a relatively long-term marker of past exposure to the virus. It generally starts to increase 2 weeks after first exposure and stays elevated for many months. The IgG test can be elevated even after the virus is gone.
The timing of elevation in these three tests often overlap in the first month of infection (see figure). Knowing how these tests related to each other can be helpful. For example, the virus test can be positive but the IgM and IgG tests negative which suggests a recent virus infection and the immune system has not had time to create the antibodies. IgM is the first antibody to respond to this virus infection and if the IgM is elevated but the IgG not elevated, it suggests an infection.
Testing is being conducted and reported in novel ways and means unfamiliar to most. The messaging of what each test is reporting, as well as taking into account our body’s ‘immune system’s time clock’ must be part of the narrative to understanding test results. Combining tests and adhering to current health guidelines is our best defense to this Coronavirus pandemic. What we learn and implement today will help us combat future viral epidemics. Difficult times often teach us the most valuable life lessons. Learning and practicing preventive health today helps to ensure healthier generations tomorrow.
Complete COVID Testing
Diagnosis of a current infection is made by clinical observation and testing. The combination of virus and antibody testing is important for confirming or excluding current or past infection.
Real-Time PCR testing is used to detect RNA from the SARS-CoV-2 virus. This testing is used to monitor for active infection, but may become undetectable with increasing time from disease onset.
Antibody levels suggest some amount of immunity or resistance to the SARS-CoV-2 virus and is also used to determine who may have been infected and not have had symptoms. Antibody test are critical for contact tracing of asymptomatic people.
ACTIVE VIRUS TESTING BY RT-PCR – $130
. Utilizes a convenient oral swab and mouth rinse to detect SARS-CoV-2 virus, the virus that causes COVID-19
. This test is highly specific to SARS-CoV-2 and is unlikely to cross-react with any other viral infection.
ANTIBODY TESTING BY CHEMILUMINESCENCE – $80
. Automated chemiluminescence antibody testing is one of the most sensitive at detecting low levels of antibodies.
. Testing is performed in a highly complex, CLIA laboratory by qualified and highly trained laboratory technicians.
. Minimizes the uncertainty of results identified in finger-stick, cartridge testing.
* Test results should not be the sole basis for the diagnosis or exclusion of COVID-19. Speak with your health care provider if you are experiencing any COVID-19 related symptoms
Prevé® offers the COVID Virus and Antibody testing at Select Labs of Marion County. Call or go online to make an appointment.
 Central Florida Health and Wellness Magazine Health and Wellness Articles of the Villages
Central Florida Health and Wellness Magazine Health and Wellness Articles of the Villages