Dr. Mark Jacobson
 This week, I am deeply moved by the loss of one of my patients. This one, in particular, left an impression on all of my staff. His relentless endearing spirit regardless of his pain and suffering, never ceased to amaze us. When his wife called with the news, we all felt as though another member of our MIT family had been lost. The solemnness passed throughout every department once again, as we tried to continue about our day, offering hope and kindness to our other patients, who look to us for diagnoses and treatments, and a little “extra attention,” that we often provide, to help them overcome their ailments. Although it is advised not to get attached, sometimes, it is impossible not to, especially if they have spent years and numerous procedures with me. Getting acquainted with my patients helps ease their anxiety. Allowing them to talk and express themselves is often something they don’t get a chance to do as they are rushed from appointment to appointment. In my practice, developing a personal relationship with patients is the norm. What kind of doctor would I be if I couldn’t provide a comforting voice, and tender touch in addition to my medical expertise? Not only do they get a lot from me, but each one unknowingly teaches me a little something which I can apply towards my other patients. The art of listening is somewhat of a dying art among physicians. Patients really deserve to be heard.
This week, I am deeply moved by the loss of one of my patients. This one, in particular, left an impression on all of my staff. His relentless endearing spirit regardless of his pain and suffering, never ceased to amaze us. When his wife called with the news, we all felt as though another member of our MIT family had been lost. The solemnness passed throughout every department once again, as we tried to continue about our day, offering hope and kindness to our other patients, who look to us for diagnoses and treatments, and a little “extra attention,” that we often provide, to help them overcome their ailments. Although it is advised not to get attached, sometimes, it is impossible not to, especially if they have spent years and numerous procedures with me. Getting acquainted with my patients helps ease their anxiety. Allowing them to talk and express themselves is often something they don’t get a chance to do as they are rushed from appointment to appointment. In my practice, developing a personal relationship with patients is the norm. What kind of doctor would I be if I couldn’t provide a comforting voice, and tender touch in addition to my medical expertise? Not only do they get a lot from me, but each one unknowingly teaches me a little something which I can apply towards my other patients. The art of listening is somewhat of a dying art among physicians. Patients really deserve to be heard.
To offer a patient therapeutic care often means to keep them comfortable by reducing and hopefully eliminating their pain. For those who are healthy but might be suffering from an injury or chronic pain, oftentimes, there is permanent healing through injections or minor surgical repairs, but then there are those who are afflicted with a terminal illness. Although I feel privileged to assist in the management of my patients during these situations, no matter how sick they have become overtime, we are never really prepared for the news of their passing. We all hope we can all live forever, but unfortunately, we can’t, and it is always a very sad day, and a feeling of loss not only for their families at home, but for those of us who have tirelessly tried to ease their suffering. The tears, hugs, smiles and laughter throughout their journey bring us close to them and their families and so it is often a family member who calls or visits to tell us unfortunate news, oftentimes seeking the support and comfort they also received when they accompanied their loved one during visits to my office.
My oncology patients come to me from many specialties. Perhaps, pain can send them to an urgent care center, who sends them to me for imaging studies, or a primary care doctor may order a CT or MRI because something hurts, a gynecologist orders a mammogram and a suspicious lesion is found. As an interventional radiologist, I can perform a biopsy and send the specimen to a lab that will establish the underlying diagnosis. If it is positive for cancer, the referring physician often consults with me to determine who is the best oncologist to treat them. Very often, the patient returns to me, and I will place a port or PICC line so the patient may receive chemotherapy or other infusion therapy. They may return for numerous followup imaging tests, and minor surgical procedures along the way. I am overjoyed when they recover and continue leading a healthy life, which is the case for many, but for others, their journey is not so simple. Some develop fluid around their lungs, called pleural effusions, or they may develop fluid in their abdomen, called ascites. Using ultrasound guidance, I can drain these fluid collections in the comfort and privacy of my center. These procedures give them relief so they will breath, sleep, eat and perform better, and can continue to live a good quality of life and not have to feel home bound.
There are many advantages to coming to an outpatient center, instead of a hospital. For one thing, it is small and personable. You will see the same doctor and staff who will develop a relationship with you, and oftentimes get to know your family members. This is important, because the same doctor will recognize minor changes in your condition that may often go unnoticed in situations where there is no such continuity of care. Outpatient centers rarely have antibiotic resistant organsims such as MRSA, VRE, (In our four years, we have had zero cases) so it is especially healthier for those who are immunocompromised. It’s also comforting to return to the same center and people, knowing what to expect! Simply to be treated in such an environment is restorative to the body and spirit, which in and of itself, is therapeutic!
MIT
352-261-5502 | mitflorida.com
facebook.com/mitflorida
The Summit Medical Park
769 Co Rd 466, Lady Lake, FL 32159
Check Also
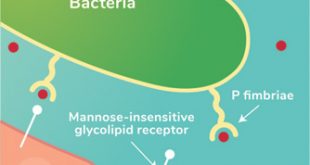
Recurrent UTIs: Addressing the Risk of Antibiotic Resistance
Urinary tract infections (UTIs) are common bacterial infections that affect millions of individuals worldwide each …
 Central Florida Health and Wellness Magazine Health and Wellness Articles of the Villages
Central Florida Health and Wellness Magazine Health and Wellness Articles of the Villages