In estimated 5% of children and 3% to 4% of adults in the United States have a food allergy.1 Allergic reactions to foods can range from local (isolated oral irritation), to systemic (hives or a life-threatening, anaphylactic reaction).1 Eight foods, or food groups, account for 90% of serious allergic reactions in the United States: peanuts, tree nuts, eggs, milk, fish, crustacean shellfish, wheat, and soy.1
This newsletter discusses different methods of testing for food allergies, including whole-food allergen testing and component testing. Food allergy testing helps predict whether it is safe to eat a certain food, or whether to avoid the food entirely.
Whole-Food Allergy Tests
In addition to clinical history, whole-food allergy tests have traditionally been used to diagnose IgE-
mediated food allergies. These tests include skin prick tests (SPTs) and blood tests (serum IgE tests) using crude extracts of food. Whole-food allergen tests (serum IgE or SPT) are very sensitive, but not very specifi c. For example, IgE responses to nuts may be directed at similar proteins from other plant or tree species and not the nut of concern.2,3 In these cases, if the nut of concern were eaten, the cross-reactive IgE would likely cause at most a mild clinical reaction. Likewise, for milk and egg, IgE responses directed toward heat-labile proteins may be associated with clinical tolerance in baked goods.2 In contrast, IgE responses directed toward heat-stable peanut-, tree nut-, milk- and egg-specific proteins are strongly linked to anaphylactic hypersensitivities.2,3
Because of these issues, whole-food allergen tests have limited value for discriminating between IgE-
sensitized and truly allergic patients.1,2 This distinction is very important clinically. Both sensitized and allergic patients have positive whole-food allergen tests (SPT or serum IgE). But sensitized individuals may not experience symptoms and may benefi t from continued consumption of the food to maintain clinical tolerance. In contrast, truly allergic patients develop symptoms immediately after ingesting the food, and subsequent ingestion may provoke more severe allergic reactions.
Food Component Tests
Food component testing involves serum IgE tests using individual protein components of the whole food, rather than crude extracts. These tests confirm whole-food IgE reactivity to suspect foods, and identify the specific protein(s) to which IgE binds.2,3
As such, they can be used to help predict patient risk for a clinical reaction when the food is eaten.2,3 When compared to whole-food SPTs and IgE tests, food component IgE tests are better able to identify patients at high risk of anaphylactic reactions to the suspect food.2,3 Examples of currently available food component tests and the interpretation of results are presented on the next page.1,3,4
How the Laboratory Can Help
Quest Diagnostics offers IgE testing for a wide range of whole foods, as well as component IgE testing for select food allergens, including peanuts, tree nuts, milk, and egg: QuestDiagnostics.com/home/
physicians/testing-services/condition/allergy/
allergen-component-testing.html.
QuestDiagnostics.com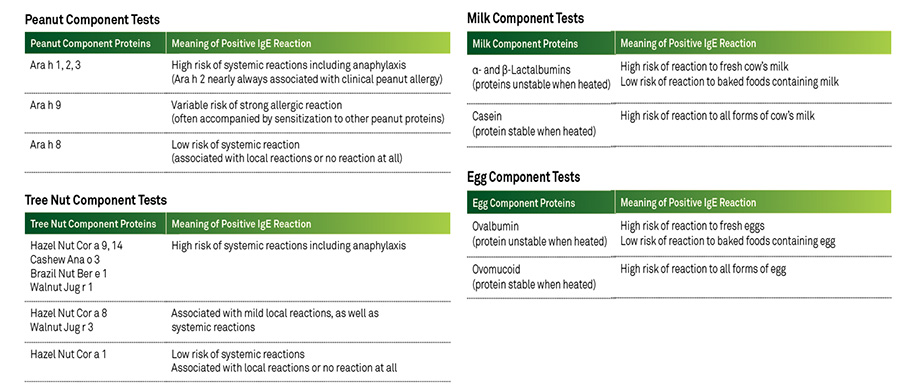
Food Allergy Diagnostic Strategy2
• Medical history and exam
• Whole allergen IgE testing or skin prick testing
• Food component IgE testing if wholefood allergy test is positive
• Oral food challenge if indicated based on clinical history and allergy test results
• Potential medical management
– Strict avoidance diet and anaphylaxis precautions during meals if allergy is present
– Modifi ed diet (ie, milk and egg only in baked goods)
– Unrestricted diet
What Does Component Testing Mean for You and Your Patients?
Patients want to know if they are truly allergic to a food. Food component IgE testing can help
you make more informed decisions about
• The likelihood that an oral food challenge will be passed
• The need for dietary restrictions
• The need to carry epinephrine
• The likelihood that a food allergy will be outgrown4
References
1. Sicherer SH, Sampson HA. Food allergy.
J Allergy Clin Immunol. 2010;125 (suppl 2):S116-S125.
2. Chokshi NY, Sicherer SH. Interpreting IgE sensitization tests in food allergy. Expert Rev Clin Immunol. 2016;12:389-403.
3. Nicolaou N, Poorafshar M, Murray C, et al. Allergy or tolerance in children sensitized to peanut: prevalence and differentiation using componentresolved diagnostics. J Allergy Clin Immunol. 2010;125:191-197.e1-e13. doi: 10.1016/j.jaci.2009.10.008.
4. Eigenmann PA. Do we still need oral food challenges for the
diagnosis of food allergy? Pediatr Allergy Immunol. 2018;29:239-242.
Check Also
Obstructive Sleep Apnea & Oral Appliances: A Solution for a Good Night’s Sleep
By Richard W. Rozensky, DDS, D.ABDSM Sleep apnea affects more than 25 million people in …
 Central Florida Health and Wellness Magazine Health and Wellness Articles of the Villages
Central Florida Health and Wellness Magazine Health and Wellness Articles of the Villages