 Diabetes, as with other health issues, can contribute to diseases of the eye, particularly if a person has untreated high blood glucose, high blood pressure and/or high blood cholesterol. Smoking may also increase the risk of eye disease. However, when caught early, diabetic eye diseases may be treated and managed so that eyes maintain health and clarity.
Diabetes, as with other health issues, can contribute to diseases of the eye, particularly if a person has untreated high blood glucose, high blood pressure and/or high blood cholesterol. Smoking may also increase the risk of eye disease. However, when caught early, diabetic eye diseases may be treated and managed so that eyes maintain health and clarity.
Diabetic Retinopathy
Diabetic retinopathy is a condition that damages the tiny blood vessels that deliver blood and nourishment to the retina, the light-sensitive layer of tissue at the back of the eye. Diabetic retinopathy affects roughly 40%-45% of adults with diabetes, although only about half know they have it. It is the not knowing that is dangerous, because, while it can be quite serious, early diagnosis and treatment of diabetic retinopathy can reduce the risk of related blindness by as much as 95%. That’s why detection is so important.
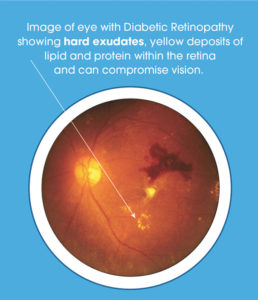
There are two types of diabetic retinopathy: nonproliferative and proliferative. Nonproliferative diabetic retinopathy, or NPDR, is a condition in which damaged blood vessels leak fluids into the retina, causing swelling and in some cases the formation of fatty deposits called hard exudates. The blood, fluid and exudates can force the macula, the part of the retina that detects light and enables central vision, to inflame or thicken, warping vision. Conversely, NPDR can force blood vessels feeding the retina to close off, starving and damaging the macula and causing blurring or darkening of central vision.
Proliferative diabetic retinopathy, or PDR, describes an advanced form of the disease, in which blood vessels in the retina become blocked, limiting blood supply and stimulating the retina to produce new blood vessels.
Regrettably, the new blood vessels tend to be weak, deformed and prone to rupture, causing scarring and cell death. These problems can cause the retina to warp or detach, creating floating or blind spots. PDR can also lead to excessive fluid build-up, elevating eye pressure and promoting glaucoma.
Diabetic Macular Edema
Diabetic Macular Edema, or DME, occurs when the bleeding or other fluid leakage caused by diabetic retinopathy causes the macula to swell. Any damage to the macula can impair central vision, which is needed to drive, read and
recognize faces. People with DME tend to rely more and more on their peripheral vision to see. It affects roughly half of all diabetic retinopathy patients.
Managing Diabetic Eye Diseases
Certainly all of this sounds scary, and it should cause enough alarm to encourage people with diabetes to take steps to preserve and protect their vision. Luckily, getting started is simple.
Get Regular Eye Exams
Adults with diabetes should schedule a comprehensive dilated eye exam once a year, or more often if recommended by your eye doctor. Your doctor will examine the systems within your eye and notice changes in their earliest stages, when treatment is easiest and most effective. Caught early and treated appropriately, nearly all cases of serious vision loss can be prevented.
Know Your Numbers
Evidence shows that people who keep their blood glucose at normal levels have significantly less risk of developing diabetic retinopathy than people who don’t. So keep track of your blood sugar and see your regular physician immediately if your levels fall outside a healthy range – it is the key to controlling diabetes instead of letting it control you. Keep an eye on your blood pressure and blood cholesterol, too, and if you presently smoke, talk to your doctor about ways to help you quit. It’s never too late to get rid of a bad habit.
Treating Diabetic Retinopathy
Controlling blood sugar and getting regular comprehensive eye exams from your ophthalmologist or optometrist are the best places to start.
From there, diabetic retinopathy can be managed with medications, corticosteroids and macular or retinal laser outpatient surgery, wherein a retinal specialist can shrink or stem leaky blood vessels, often right there in his or her office using a local anesthetic.
When diabetic retinopathy and related DME advance to a level where they affect or threaten vision, they can be treated using injectable medication called anti-VEGF (vascular endothelial growth factor). This therapy blocks the VEGF protein that encourages abnormal blood vessels to form. Blocking VEGF is an effective way to reduce these vessels and excess retinal fluid. Typically, patients may require monthly injections for 6 months, after which they are needed less and less as the disease becomes under control. This is often the first line of defense against diabetic retinopathy and DME.
Another effective medication is corticosteroid injection or the implantation of a short-term or long-term corticosteroid in the eye that releases a sustained dose of medication over time. Your Lake Eye doctor will describe the suitability of this treatment for your particular case.
Less often, patients may require macular laser surgery to seal off leaking blood vessels. Most people respond favorably after just one treatment session, which may or may not be performed in conjunction with drug therapy.
Very serious bleeding cases may require a procedure called a vitrectomy, which is the removal of the vitreous gel in the center of the eye, along with any scar tissue. It is also used to treat a detached retina. Should bleeding be severe enough to warrant vitrectomy, your doctor will refer you to a specialist.
Again, while all of this may seem a bit overwhelming, diabetic retinopathy and DME are treatable conditions. With some dedication to your health and vision, and regular appointments with your eye doctor, you can help keep your eyes healthy and functioning long into the future.
Lake Eye Associates
352-750-2020
www.lakeeye.com
 Central Florida Health and Wellness Magazine Health and Wellness Articles of the Villages
Central Florida Health and Wellness Magazine Health and Wellness Articles of the Villages



